PARENTS / CAREGIVER
Parenting has its ups and downs when your child (or children) are healthy. But when your child has an illness or injury, it becomes a more difficult balancing act. What can help is gaining a better understanding of your children’s reactions and establishing routines.
Parenting has its ups and downs when your child (or children) are healthy. But when your child has an illness or injury, it becomes a more difficult balancing act. What can help is gaining a better understanding of your children’s reactions and establishing routines.
 Taking care of a child with an illness or injury poses unique challenges, especially if you have other children at home. You will have your own fears and worries, and so will the rest of your family. Everyone reacts and copes in different ways. It may be hard to understand why or stress your relationships. However, it is very normal.
Taking care of a child with an illness or injury poses unique challenges, especially if you have other children at home. You will have your own fears and worries, and so will the rest of your family. Everyone reacts and copes in different ways. It may be hard to understand why or stress your relationships. However, it is very normal.
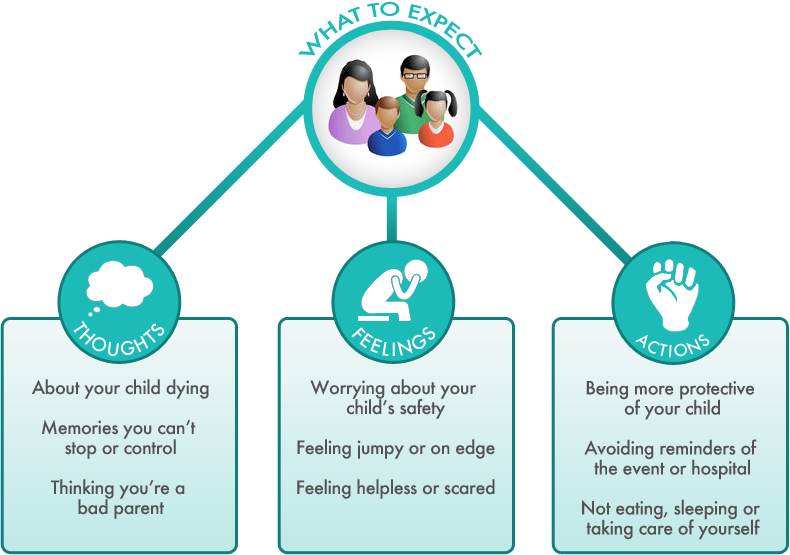
You might find yourself having the following thoughts and feelings, or doing the following actions:
Even though these reactions are common, if they begin to get in the way of your daily life or last more than one month, it might be a sign you could use extra help. You can talk to your doctor, a clergy member, or a counselor for help in coping, and check out “Therapy for Your Child and You” for additional information and support.

Taking care of a child with an illness or injury poses unique challenges, especially if you have other children at home. You will have your own fears and worries, and so will the rest of your family. Everyone reacts and copes in different ways. It may be hard to understand why or stress your relationships. However, it is very normal.
You might also find yourself having the following thoughts and feelings, or doing the following actions:
Even though these reactions are common, if they begin to get in the way of your daily life or last more than one month, it might be a sign you could use extra help. You can talk to your doctor, a clergy member, or a counselor for help in coping, and check out “Therapy for Your Child and You” for additional information and support.
Supporting Your Entire Family
No one expects an illness to happen to their child. When it does, it can be a traumatic and overwhelming experience. It’s common for you and your entire family to feel upset, scared or worried. Honest communication, establishing routines and gaining a better understanding of your children’s reactions, based on age, can make it easier to cope.
Below are some tips to help you manage. You can also visit the Resources page for additional information and support.
- A new diagnosis can be incredibly scary and overwhelming. It’s hard to know what to do first. Take things one step at a time and lean on your medical team and social supports. It can also be helpful to sit down and create an action plan to organize your thoughts and priorities. Find out how, and get additional advice, by reading What to Do When Your Child is Diagnosed with Cancer or a Serious Illness.
- While your children may not be aware of what is going on, they pick up on a lot.
- Try not to get frustrated when your child regresses. This is very normal.
- Continue to parent your children, but keep in mind realistic expectations.
- For your other children (siblings), if they feel scared, let them know it is okay to come to you.
- Reassure your children that the feelings that they are feeling are normal, and help them work through them. Fear and anxiety are especially common, but can be difficult for both your child and you. One of the best things you can do is listen to their concerns, help them name their feelings and support them in identifying healthy stress techniques that fit their interests in their age. You can also get more tips on helping your child manage fear and anxiety here.
- Make time to connect with your significant other to help keep your relationship strong.
- Siblings may feel jealous or hurt when a lot of attention is given to their sibling with an illness or injury. Try to make time for them one-on-one and enlist your friends and family to help. Teach them that they can still have fun by doing family activities such as hospital slumber parties, movies or playing games. For more information on how to support siblings, visit the Coping Tips for Siblings page.
Parenting at the Hospital or Clinic
Hospitals and/or clinics can be strange and scary places for both you and your child. You might not know where to find things or who to ask for help. When your child is in the hospital, it’s normal to feel sad, angry or even guilty the first couple times you see your child in a hospital bed, hooked up to machines, or feeling sick. You may feel upset, or even helpless, as your role of caregiver to your child changes over the course of their illness or hospital stay.  Keep in mind, you are the expert on your child. You know how best to comfort them, and it’s okay to let the hospital staff know what works. Most will be happy to accommodate you. However, there may be times you need to advocate for your child at the doctor’s. Persistence is key, as is preparation, confidence and finding allies amongst supportive hospital staff.
Keep in mind, you are the expert on your child. You know how best to comfort them, and it’s okay to let the hospital staff know what works. Most will be happy to accommodate you. However, there may be times you need to advocate for your child at the doctor’s. Persistence is key, as is preparation, confidence and finding allies amongst supportive hospital staff.
Depending on the medical equipment needed, you may not be able to put your child at ease. In this case, it can be helpful to ask the doctors and nurses for advice. You can also work with the nurses to create a home-like setting in the hospital room. Bringing pictures or favorite items, like a toy, book, or pillowcase, can make the room more comforting.
Remember whether in the hospital or not, you are a source of strength and a role model for your child. Even though it may be hard at times, answering your son or daughter’s questions, being honest about what is happening, and reassuring them that the hospital staff is doing everything they can to help will put your child’s fears and worries at ease.
The Hospital Environment:
- Think about what makes your child comfortable. (Ex: They do not like hospital pajamas so you may bring some from home.)
- Keep your child’s toys in organized tubs and bring them to the hospital.
- Boundaries are important. It is okay to say no to visitors.
- If your child is not up to having visitors, suggest they meet you in the hospital cafeteria instead of the room.
- If you have to stay at the hospital, bring food from home.
- Depending on their age, include siblings in appointments and hospital stays. Long hospital stays can be lonely and isolating for many family members.
Parenting During Procedures:
- Be honest with your child. If a procedure will hurt, let them know.
- When your child has to fast (not eat) for a procedure, it is helpful if you fast too. Have on hand the foods that your child would want, once they are able to eat again. If you do have/want to eat when your child is not able to, leave the room so they do not see you eating.
- You can find additional tips for helping your child, based on their age, on the Children page.
Reaching Out for Help:
- Utilize the hospital staff, such as a child life specialist and music therapist. These therapies can be good, even for toddlers.
- Seek what external help exists while you are in the hospital. (ex: Ronald McDonald House, Ronald McDonald Room, Social Work Department for meal or parking assistance).
- Consider having a close friend or family member take notes during meetings about your child’s care. All the information can be overwhelming.
Keep Track of Everything!
- Keep a notebook with details of conversations with doctors, medicines, etc.
- Write down any questions that you may have for hospital staff.
- Keep a notebook for other record keeping – gifts, meals, or services for thank you notes.
Leaving the Hospital
The day your child is discharged from the hospital can be filled with many mixed emotions. You may feel happy, relieved, and excited to have your whole family back at home again, but it’s common to also feel scared, nervous, or not ready to care for your child without the hospital staff. It’s helpful to talk to your son or daughter’s doctor or nurse about what you can expect at home and who to call if you need help.
Questions to Ask Before Discharge:
- What medicines will my child need to take at home?
- How often does my child need to take these medicines? For how long?
- Is there anything my child isn’t allowed to do? For how long?
- Are there foods my child shouldn’t eat? For how long?
- What medical care do I have to give my child at home? How often?
- What follow-up appointments do I need to make?
After returning home, everyone in your family will need time to re-adjust. You may find that you will react and cope with this adjustment differently than your child and other family members. Remember to be patient with everyone – including yourself! It may also be helpful to review common reactions by age, as well as tips for helping your child cope, on the Children page.
Tips to Set Up a Routine
As you and your family adjust to life at home, it’s important to get back to a routine and to renew relationships. Getting back to a routine can help your child, family and yourself feel safe, organized, and in control again. While it may be tempting to relax any house rules, it is better to keep them the same.
- Keep the same morning routine and breakfast time. This makes starting the day easier.
- Set up a family check-in routine. This can happen in the morning to help plan the day, or any time that works for your family.
- Don’t forget about playtime! Setting aside a set time for your child and family to have fun is important. Playing your favorite games, reading, drawing, or watching movies are all great ways to have fun!
- Just like in the morning, keep to the same night routine. Have a dinner and bedtime routine to help everyone relax at the end of the day. Dinnertime can be a great time to talk about what happened during the day. Taking a bath or reading a bedtime story can help your child unwind and go to sleep easier.
- Remember to schedule time for yourself! Set time to check-in with yourself each day. Take time to breathe, relax, and think about what is going well in your life at the moment.
Managing School
Sometimes an illness or injury requires a child to miss school for an extended period of time. Others may result in a brief absence. Regardless, many parents worry about how their child will keep up with academics. Luckily teachers, as well as school nurses, guidance counselors and other school staff, are often happy to help.
Below are a few tips to support your child’s ongoing learning and manage the transition upon their return. You can also read a more detailed review of the back to school process on our blog.
While Your Child Is in the Hospital or at Home
- Keep your child’s school informed of your family situation. Your child’s teacher, school nurse or guidance counselor can be all be advocates to ensure all your children receive the additional emotional care they may need.
For elementary school students, start with your child’s classroom teacher, and ask him or her about other school resources such as the school nurse or guidance counselor.
For middle and high school students, you might start with the school nurse or guidance counselor assigned to your child. If no nurse or counselor is available, talk with the principal or vice-principal.
- Speak with your child’s school and inquire about any assignments that they can do while in the hospital or at home. Check also with your child’s healthcare team to see what hospital resources may exist. Many children’s hospitals will have services to support schoolwork for kids with longer admissions.
- Well ahead of your child’s return to school, set up a meeting with the school to discuss any special arrangements or additional support that may be needed.
- Your child may be eager to return to school or nervous to do so after their illness or injury. Take time to prepare your child, including talking with them about any feelings they may have and their concerns.
- If you have other children who are in school during this time, make sure to let their teacher(s) or school counselor know about what is happening in the family. The School Sibling Support Form can be a great place to start. Help siblings think through how they want to respond to any questions about their brother or sister as well.
When Your Child Returns to School
- Maintain open communication with the school and make a plan with your child’s teachers. Work with them to figure out a manageable way for staying in touch about how they are adjusting.
- Help your child identify a specific person to speak with if they have any worries or concerns. Talk with that person or, if your child is older, help them to talk with that person to ensure that they know of the plan and are available. (Ex: teacher, counselor or coach)
- Speak to your contact at the school to discuss any medications your child may be take and side effects that they may see at school. You should also discuss problems to watch for, an emergency management plan, and any precautions that need to be taken or information you need to know (ex: another student develops chicken pox or some other illness that might be a problem for your child).
- Some treatments have late-effects that can impact your child’s stamina, concentration, vision/hearing, digestion and more. Be sure the school is aware of this and can monitor any changes that may cause concern. You may also want to discuss if your child 504 plan or Individualized Education Plan (IEP).
- Be sensitive to the needs of siblings attending school. See additional tips for helping them cope with their unique situation on the Sibling Coping Tips page.
- Ask your child’s healthcare team about any school re-entry programs that may be offered to help transition your child back to their classroom. Your child may have mixed emotions when returning to school and a re-entry program can help ease those fears. You may also want to ease back into school slowly, with your child beginning by attending only a few days a week.
- Prepare your child for any questions they may receive from classmates or staff. Help them think through how they want to respond if classmates ask about what happened to them, why they were out of school, whether their illness is something that others can “catch” (i.e. contagious), etc. If your child has had visible changes in their appearance or has activity restrictions, think about how to talk about those things as well. Suggested phrases and additional tips can be found in the “Preparing Your Child to Address Questions” section below and our How to Help Your Child Answer Questions article.
Additional Resources
- KidsHealth – Balancing Academics and Serious Illness
- Healthcare Toolbox – School Concerns
- Digging Deep – Returning to School Following Treatment for Serious Illness
- American Cancer Society – Helping Your Child Manage School During Cancer Treatment
- American Cancer Society – Returning to School After Cancer
Preparing Your Child to Address Questions
After the injury or illness your child may be nervous, embarrassed or anxious to go out in public or return to school. Even if your child’s physical appearance may not have changed, he or she may just feel different. Talking about scenarios that could happen, and then practicing responses, can give them more confidence. Additional ideas and advice for helping your child answer questions about their illness can be found here.
What Happened to You?
- Discuss with your child what they can say if they want to answer, such as,“I had to go the hospital because I got hurt. The doctors and nurses helped my body. I’m feeling better now.”
- Your child could talk briefly about their illness or injury.
• “I have cancer, and I had to go to the hospital for a while so the doctors could help my body fight it.”
• “I had to have a transplant because my kidneys weren’t working so great. Now I am feeling a little bit better.” - If your child does not want to talk about it at the time, they can say that politely and then change the subject, or suggest something else to do together.
• “I don’t really want to talk about it right now. Let’s [other activity].”
• “Thanks for asking. I don’t feel like talking about it right now. [Then start a conversation about something else.]”
If Someone Is Staring
Your child’s appearance may have changed due to their illness or injury. It is important to talk about what to do if your child notices someone staring.
- People often stare because they are curious. Your child could:
• Smile back.
• Say “Hi” – this often stops the person who is staring.
• Start a conversation such as, “This store is really busy today”, or “It’s nice the sun is out today”.
• Come up with a witty comeback such as, “Haven’t you ever seen a rock star before?”.
If Someone Is Making Fun of Them, Name-Calling or Being Rude
- Help your child rehearse things to say INTERNALLY, to him or herself, to feel strong and positive.
- Your child could walk away and not address the insult.
- If it is appropriate or necessary to say something, help your child figure out what works for them. Trading insults or being mean back is not likely to be helpful. Try coming up with positive responses.
• “I’ve been sick, but I’m feeling pretty good about myself today.”
• “I don’t like it when you say that. You wouldn’t like it if people made fun of you.” (Speaks about the effect on the child on the receiving end.)
• “Saying those things is mean.” (Describes behavior, not the person)
Remember: Teach your child to leave the situation if they are very uncomfortable or feel they are in danger, and to tell someone immediately that they are being picked on.
Understanding Medical Terms
What did they say? When a doctor speaks it may sound like a different language. All those terms, what do they mean? It is hard to focus or ask questions when you do not understand the words. If you find yourself listening to the doctor speak, and do not understand what they are saying, ask the doctor to stop so you can ask questions or ask to have the information re-explained using different words.
You may also want to:
- Write down terms that you do not know or ask the doctor to write it down for you so you can look it up later.
- Did the doctor use letters instead of a word, like MRI, CT or EEG? Ask them what those letters stand for and to explain further.
- If you have a doctor meeting scheduled, you may want to think about having a family member present to take notes. This will allow you to focus on what the doctor says and reflect back on the notes at a later time to see if you have additional questions.
- Ask for other materials or handouts to help you better understand your child’s diagnosis and treatment.
- Use the teach-back method. Listen to what the doctor says, then repeat it back so you can confirm that you have the information correct.
- If needed, ask for a little time to think about everything. Request a follow up meeting to discuss any additional questions or make decisions on treatment options.
What is Palliative Care? (Is My Child Dying?)
Palliative care, while sometimes occurring at the same time as end of life or hospice care, does not mean that your child is dying. Rather, they are there to help them live a fuller life.
Palliative care teams are often brought in when a child is diagnosed with a life changing illness or injury and can help manage some symptoms such as pain, nausea or anxiety. This team of professionals is meant to work alongside the primary care team and provides extra support to the entire family.
Key members of your palliative care team may include:
- Physician
- Nurse
- Nurse Practitioner
- Social Worker
- Child Life Specialist
- Chaplain
- Other complementary services such as Art Therapy, Music Therapy, Dance/Movement Therapy or Pet Therapy
If you have any questions about your palliative care team, or would like to request additional services, talk to your child’s physician or child life specialist.
Pill Swallowing
Pills can be a part of many medical treatments – whether it’s for cancer or the flu. While some medicines can be administered in liquid form or crushed up, many others are only available as a pill. Swallowing these pills can be a source of anxiety for many children and adults.
If your child is afraid or believes they cannot swallow a pill, speak with their healthcare provider to see if there is another way to take the medicine. If not, they may have tips to help your child learn. Some hospitals and clinics also have professionals who specialize in teaching children how to swallow pills, such as child life specialists or nursing staff.
Below are additional tips to help your child learn.
Practicing Pill Swallowing
For most, learning to swallow pills is possible but it will take practice. As a parent, it is important to be a source of positive encouragement to help your child learn this new skill. While there are many tips to help swallow pills, your child may have to practice to find what works best for them. Try to limit practice sessions to 20-30 minutes at a time and be sure to cheer them along the way.
-
- Speak to your child’s doctor of pharmacist to identify the size of the pill your child will need to swallow.
- Gather candies in a variety of sizes to practice swallowing. Not into using candy? Try rolling soft bread into balls instead.
• Cake sprinkles or Nerds
• Mini M&Ms
• Tic Tacs
•M&Ms, Skittles, Reece’s Pieces
• Mike and Ikes or empty gel capsules (check with your doctor or pharmacist for availability)
- Start with the smallest piece and work up to the desired pill size. Have your child place the “pill” on the back of their tongue, take a sip of water or juice and then swallow.
- As they practice, experiment with different methods.
• Some people choose to look forward while swallowing their pills, while others put their chin up, chin down or turn their heads sideways to help.
•Try a straw or a sippy cup.
•For some people, swallowing a pill with juice or water does not work. Find a food such as pudding, yogurt, banana or applesauce to put the whole pill in for your child to swallow. (Be sure not to crush up the medicine as it may not work as well.)
- Always end a practice session with a success, even if it means going down a size in the candy or bread.
- If you find that your child is still having trouble swallowing pills, speak to your doctor about additional help or referrals.